Freedom from glasses starts here.
Freedom from glasses starts here.
Cataracts are a clouding of the eye’s natural lens. As the lens becomes less clear, vision can turn blurry or hazy, lights can feel harsher, and night driving often becomes difficult because of glare and halos. Cataract surgery treats this by removing the cloudy natural lens and replacing it with a clear intraocular lens (IOL), with the goal of improving clarity, contrast, and everyday visual comfort.
Cataract surgery treats this by removing the cloudy natural lens and replacing it with a clear intraocular lens (IOL), with the goal of improving clarity, contrast, and everyday visual comfort.
A cataract forms when the natural lens, which sits behind the coloured part of the eye (the iris), loses its clarity. This usually happens slowly over time, and symptoms can creep up in a way that feels like you just “need stronger glasses”.
What causes cataracts
Age-related changes (most common): Most cataracts develop as part of normal ageing. The proteins in the lens change over time, which can reduce transparency and create scatter of light.
Medical and environmental factors (high level): Cataracts can also be influenced by medical conditions such as diabetes, long-term steroid use, previous eye injury or surgery, and cumulative UV exposure. If you have diabetes-related eye concerns, it is worth reviewing diabetic retinopathy as part of your overall eye health planning.

Cataract symptoms vary, but common ones include:
If you want a deeper overview of cataracts as a condition, see cataracts.
When cataracts become a problem
Cataracts become a practical problem when vision starts to interfere with daily life, such as reading, using screens, recognising faces at a distance, driving safely (particularly at night), or doing detailed work. For many people, glare and reduced contrast are more disruptive than “blur” alone.

Cataract surgery is usually recommended when the cataract is affecting your quality of life and glasses are no longer giving useful improvement. The decision is personal, and it is based on what you need your vision to do.
Common reasons people decide it is time include:
No. Cataracts do not need to be “ripe” or fully mature before surgery. Modern cataract surgery is typically planned around how much the cataract is affecting your function, plus the health of your eye and the safety of proceeding.
Sometimes cataract surgery is recommended for medical reasons beyond day-to-day blur, for example:
If eye pressure or optic nerve health is part of your care, your specialist may also consider factors linked to glaucoma during planning.
Cataract surgery is a precise procedure performed through a small incision. The aim is to remove the cloudy lens safely, then place an artificial lens implant that stays in the eye permanently.
A typical cataract operation includes:
Most cataract surgery is performed under local anaesthetic eye drops, often with sedation offered depending on your needs and the clinic set-up. Your surgeon will explain what you will feel and what you will not feel, and will tailor comfort measures to you.
The surgical time is usually short, but your total time at the clinic is longer because of preparation, checks before surgery, and monitoring afterwards. You should plan for someone to take you home.
Lens choice is one of the most important parts of planning because it influences how often you may still use glasses afterwards. No lens is “best” for everyone. The goal is to match lens choice to your eyes and how you live.
Monofocal lenses
Monofocal lenses provide clear focus at one main distance, usually set for distance vision. You may still need glasses for near tasks such as reading. Some people choose monofocal settings that prioritise near vision instead, but that usually means needing glasses for distance. The trade-off is discussed carefully during planning.
Multifocal and extended depth of focus lenses
Multifocal and extended depth of focus lenses can reduce glasses dependence by providing a broader range of focus, but they are not suitable for everyone. Some people are more likely to notice night glare or halos with these lenses, and certain eye conditions can reduce satisfaction. If you are considering these options, the multifocal edof lenses page can help you understand the broad categories and what they are designed to do.
Toric lenses for astigmatism
Toric lenses are designed to correct astigmatism at the time of cataract surgery. This can improve unaided distance vision for suitable candidates and reduce the need for glasses to correct astigmatism after surgery.
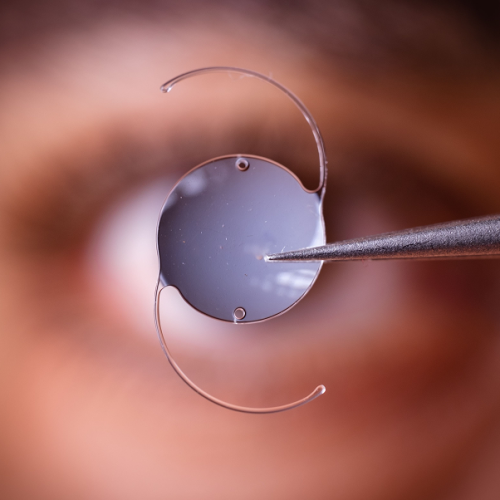
Lens selection is based on:
Cataract surgery can improve clarity and can also be planned to reduce refractive error, but it is not the same as elective laser vision correction.
If you have had laser vision correction in the past, cataract surgery is still possible, but it requires extra planning. Special measurements and lens calculations may be needed to improve accuracy, and your surgeon will discuss what level of predictability is realistic for your situation.
Cataract surgery treats a cloudy natural lens and replaces it with an artificial lens. Laser procedures reshape the cornea to correct refractive error while keeping the natural lens in place. If you are comparing pathways, laser eye surgery explains how corneal laser correction differs and who it tends to suit.
Astigmatism can be corrected during cataract surgery in several ways, depending on what is appropriate for your eye. Toric lenses are a common option. Some surgeons may also use corneal relaxing incisions in selected cases, depending on measurements and surgical planning.
Preparation focuses on choosing the right lens power, checking overall eye health, and confirming it is safe to proceed.
Your pre-op appointment usually includes:
Cryotherapy uses a freezing probe applied to the outer eye wall to create a similar sealing scar. It may be used in specific situations, such as when laser access is limited or where the tear location makes freezing more suitable.
Medication advice is individual. Blood thinners, diabetes medications, and other prescriptions may need a tailored plan around surgery day. Do not stop prescribed medication without medical advice. Your surgeon and anaesthetist (if involved) will guide you based on your health needs.
You may be given fasting instructions if sedation is planned. Arrange transport home, and plan a quiet first day. Many people find it helpful to organise meals, help at home, and time off work ahead of time so recovery is less stressful.
Most people recover smoothly, but the eye still needs time to settle. Following instructions matters because it reduces the risk of infection and helps vision stabilise.
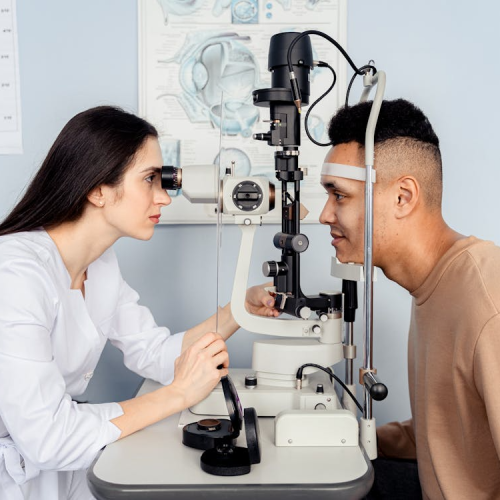
It is common to notice:
Pain that is worsening, sudden vision drop, or increasing redness should be treated as urgent and should be reported promptly.
Most patients use a combination of drops after surgery, commonly including an anti-inflammatory and an antibiotic (or equivalent regimen). Drops help reduce inflammation and lower infection risk. Your clinic will provide clear instructions specific to your case.
General guidance often includes:
Driving should only resume once your vision is safe and you have been cleared at follow-up.
Post-op checks are important because they allow your surgeon to confirm healing, check eye pressure, review the cornea and lens position, and address dryness or inflammation early. These visits also guide when it is safe to return to normal activities.
Cataract surgery often improves vision quality in a way that glasses cannot, because the issue is lens clarity rather than lens power alone.
Visual improvements most patients notice
Many patients notice:
Will I still need glasses
It depends on the lens chosen and your visual goals. Monofocal lenses often mean glasses are still needed for near tasks. Premium lens options can reduce glasses dependence for some people, but they come with suitability requirements and trade-offs that should be discussed clearly.
How long does a cataract lens last
Intraocular lenses are designed to be long-lasting and do not “wear out” like a natural lens can. Some people develop a cloudy membrane behind the lens implant months or years later, which can feel like the cataract has returned, but it is a separate issue and is treatable.
Good cataract outcomes start with good planning. Lens selection is matched to your eyes and lifestyle, with clear discussion of what is realistic for your vision goals.
Accurate measurements, careful surgical technique, and a structured follow-up plan all contribute to safety. Your surgeon will explain the steps taken to reduce risk and support predictable healing.
Aftercare matters just as much as surgery day. Follow-up visits, drop guidance, and access to support if symptoms change are key parts of safe recovery.
When cataracts are affecting your quality of life, work, reading, or driving safety, and glasses are no longer giving useful improvement. The timing is based on impact and eye health, not waiting for the cataract to become “mature”.
Most patients feel pressure and awareness rather than pain during surgery, because the eye is numbed. Mild irritation or scratchiness afterwards is common and usually improves over the first few days.
Do not drive on the day of surgery. Driving can resume once your vision is safe and you have been cleared at follow-up. Timing varies between patients.
The cataract itself does not come back because the natural lens has been removed. Some people develop posterior capsule opacification later, which can blur vision again, and it is commonly treated with a quick laser procedure.
A toric lens is an intraocular lens designed to correct astigmatism. Whether you need one depends on how much astigmatism you have and your goals for glasses independence.
“Secondary cataract” usually refers to posterior capsule opacification, where the capsule behind the lens implant becomes cloudy. It is typically treated with YAG laser capsulotomy.
It can reduce dependence on glasses, especially with careful planning and the right lens choice. Some people still need glasses for certain tasks, particularly near work, depending on the lens selected and individual visual needs.
Rediscover clearer vision
Rediscover clearer vision
Location: G11-12/566 St Kilda Road, Melbourne VIC 3004
Phone: (03) 9070 0955
Fax: (03) 9978 9426
E-mail: info@cityeyesurgeons.com.au
Copyright © 2025 City Eye Surgeons. All rights reserved. Privacy Policy.