Freedom from glasses starts here.
Freedom from glasses starts here.
What is retinal detachment
Retinal detachment means the retina has separated from the back wall of the eye. This separation reduces oxygen and nutrient support to the retina, which is why timing is so important.
Why the retina is critical for vision
The retina works like the “film” or sensor in a camera. It captures light and converts it into signals that travel through the optic nerve to the brain, where those signals become vision. When the retina is healthy and attached, it can do its job properly.
What happens when the retina detaches
When the retina detaches, the affected area stops functioning normally. The vision symptoms depend on which part is detached. A detachment in the peripheral retina may start as a shadow from the side, while a detachment involving the macula can cause central blur, distortion, or a major drop in vision.
Retinal tear vs retinal detachment
A retinal tear is a break in the retina. A retinal detachment occurs when fluid passes through that tear (or hole) and lifts the retina away from the back of the eye. Not every tear progresses to a detachment immediately, which is why early assessment is so important.
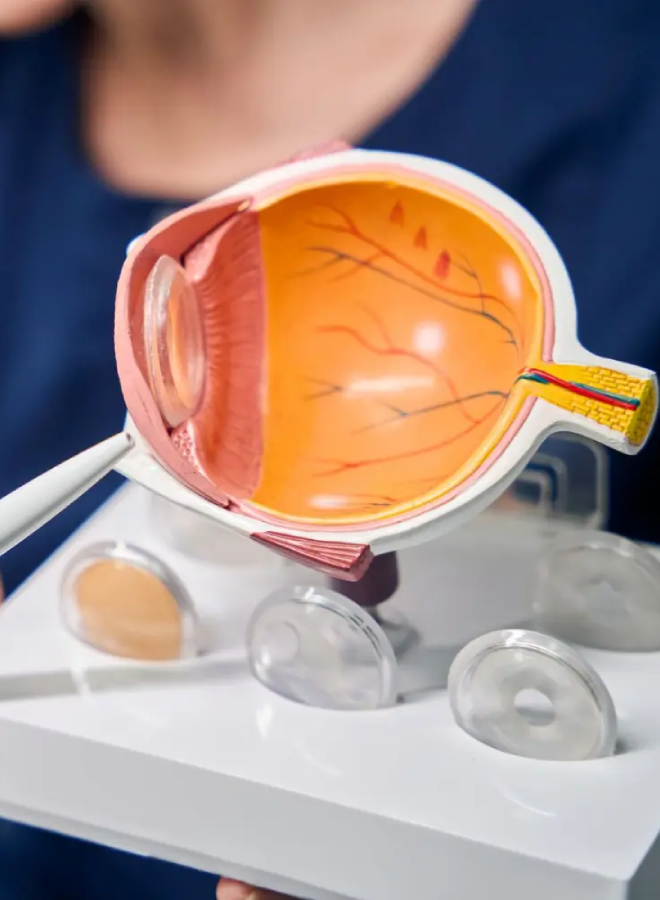
Retinal detachment is often painless. The warning signs are visual, and they can progress quickly.
Floaters can look like spots, cobwebs, or strands drifting across vision. A sudden shower of new floaters, especially if they appear all at once, can be a warning sign of a retinal tear or bleeding inside the eye.
A shadow, veil, or curtain that moves across vision from the side, top, or bottom is a classic symptom of retinal detachment. This can expand as the detachment progresses.
If you suspect a retinal detachment, do not wait to see if it improves. Early assessment is the safest approach.
Call the clinic immediately and explain your symptoms. If you cannot be seen quickly, attend an emergency department for urgent eye assessment. You can reach the team via contact us for urgent guidance on the next step.
Retinal detachment is not one single condition. The cause influences how it is treated.
Rhegmatogenous retinal detachment
Tractional retinal detachment
Exudative (serous) retinal detachment
Some people have a higher chance of retinal tears and detachments. Knowing your risk helps you act quickly if symptoms appear.
High myopia and peripheral retinal weakness
Higher levels of short-sightedness are linked with a longer eye shape and thinner peripheral retina. This can increase the risk of tears and detachments, especially if symptoms appear suddenly.
Previous eye surgery or eye injury
Previous eye surgery, especially cataract surgery, can increase detachment risk in some patients. Eye trauma can also cause tears or detachments, sometimes immediately and sometimes later.
Family history and previous detachment
If you have had a detachment in one eye, or there is a family history, your risk can be higher. Ongoing monitoring becomes more important in these cases.
Diabetic eye disease and other retinal conditions
Advanced diabetic eye disease can lead to tractional detachment. Other retinal conditions may also raise the risk of tears or scarring.
Diagnosis is based on a careful examination of the retina, often with imaging support.
A dilated eye exam allows the specialist to examine the retina, including the far periphery where tears often occur. The goal is to identify tears,holes, areas of weakness, and whether any detachment is present.
OCT (optical coherence tomography) may be used to assess whether the macula is involved and to document retinal structure. Other imaging may be used to support diagnosis and monitoring.
If the view to the retina is blocked by bleeding, dense cataract, or other media opacity, an ultrasound can help detect a detachment and guide urgent treatment decisions.
Treatment depends on whether there is a tear only, a small detachment, or a more complex detachment. The aim is to seal tears, reattach the retina, and reduce the risk of recurrence.
If there is a tear or hole without a detachment, laser retinopexy can be used to create a protective seal around it. The laser creates a controlled scar that helps “spot weld” the retina to the underlying tissue to reduce the chance of fluid passing through and causing a detachment.
Cryotherapy uses a freezing probe applied to the outer eye wall to create a similar sealing scar. It may be used in specific situations, such as when laser access is limited or where the tear location makes freezing more suitable.
Pneumatic retinopexy involves placing a gas bubble inside the eye to help press the retina back into place, usually combined with laser or cryotherapy to seal the tear. Positioning is critical, and this approach is only suitable for selected detachments based on tear location and detachment features.
A scleral buckle is a band placed around the outside of the eye to support the wall of the eye and help close the tear and reduce vitreous traction. This can be helpful in certain detachment patterns, including some in younger patients.
Vitrectomy involves removing the vitreous gel to relieve traction on the retina, reattaching the retina, and sealing the tear. Gas or silicone oil may be used to support the retina during healing. The choice of tamponade depends on the type and complexity of detachment and the surgeon’s plan.
Treatment depends on whether there is a tear only, a small detachment, or a more complex detachment. The aim is to seal tears, reattach the retina, and reduce the risk of recurrence.
Retinal detachment treatment is time-sensitive. Planning focuses on protecting the macula and reducing complications.
Timing often depends on whether the macula is still attached (macula-on) or already detached (macula-off). When the macula is still on, treatment is usually more urgent because preserving macular attachment improves the chance of maintaining central vision. If the macula is off, surgery is still important, but visual recovery can be more limited and may take longer.
Depending on the procedure and your health factors, treatment may be performed as day surgery or may require admission. Anaesthetic options vary and can include local anaesthetic with sedation or general anaesthetic, depending on the procedure and what is safest and most appropriate.
If a gas bubble is used, you may be asked to maintain face-down positioning or a specific head position for a set period. Positioning requirements depend on the tear location and the type of repair performed. Your surgeon will give clear instructions for your specific case.
If a gas bubble is placed in the eye, you cannot fly or travel to high altitude until the bubble has fully resolved. Altitude changes can cause dangerous rises in eye pressure. Driving is often restricted until your vision is safe and you have been cleared. Return-to-work timing depends on the procedure, your vision in each eye, and the type of work you do.
Recovery and vision outcomes vary widely. The type of detachment, whether the macula was involved, and how quickly treatment occurred all play a role.
How long recovery takes
Healing time varies by procedure. Some people notice gradual improvement over weeks, while others may take months to reach their most stable vision. If silicone oil is used, additional surgery may be needed later to remove it, depending on the surgeon’s plan.
What vision improvement looks like
Vision may improve gradually after reattachment, but it may not return to what it was before the detachment. Some people notice persistent distortion, reduced contrast, or blurring, especially if the macula was detached. The goal of treatment is to save vision and stabilise the retina, even when perfect vision cannot be restored.
Follow-up and monitoring
Follow-up checks monitor retinal stability, inflammation, and eye pressure. In some cases, cataract progression can occur after vitrectomy, and this is monitored over time. If you have ongoing eye care with the clinic, it may be helpful to review our doctors to understand the team involved in assessment, treatment planning, and follow-up.
When symptoms are urgent, care needs to be decisive, well-coordinated, and followed up properly.
Retinal symptoms need timely triage and same-day assessment when warning signs are present. A clear pathway helps you get the right examination quickly.
Accurate diagnosis depends on careful peripheral retinal examination and appropriate imaging. Where surgery is required, treatment planning is based on the detachment type, macula status, and the safest repair
strategy.
Aftercare instructions and follow-up visits are essential to reduce complications and monitor stability. You will be given clear guidance on positioning (if required), drop use, restrictions, and warning signs.
Retinal detachment is treated urgently. Timing depends on whether the macula is involved and the detachment features, but same-day assessment is recommended when warning signs appear.
No. Flashes and floaters are often caused by normal vitreous changes, but they can also be a warning sign of a retinal tear or detachment. Because it can be hard to tell the difference without an exam, new or sudden symptoms should be assessed promptly.
A retinal tear usually does not “heal” in a reliable way on its own. Treatment such as laser or cryotherapy is often used to seal the tear and reduce the risk of detachment, depending on the tear type and symptoms.
Some people regain strong vision, while others have lasting blur or distortion, particularly if the macula was detached. Visual recovery can continue for months, and the main aim is to reattach the retina and protect as much vision as possible.
Yes, it can. Risk is higher if you have had a detachment in one eye, have high myopia, or have certain retinal conditions. Ongoing monitoring is important if you are higher risk.
If a gas bubble is placed in the eye, flying or high-altitude travel can cause a dangerous rise in eye pressure. You can only fly once the bubble has fully resolved and your surgeon confirms it is safe.
Rediscover clearer vision
Location: G11-12/566 St Kilda Road, Melbourne VIC 3004
Phone: (03) 9070 0955
Fax: (03) 9978 9426
E-mail: info@cityeyesurgeons.com.au
Copyright © 2025 City Eye Surgeons. All rights reserved. Privacy Policy.