What to expect from glaucoma treatment
Treatment depends on your prescription, symptoms, corneal shape, and lifestyle goals. Some people want the sharpest possible correction for work and driving, while others are mainly trying to reduce the hassle of glasses or contacts.aGlaucoma care is a long-term plan, not a one-time fix. The focus is stability, protecting the optic nerve, and catching progression early if it occurs.
A “safe” pressure is different for each person. Your target is based on optic nerve health, visual field results, rate of change (if any), and individual risk factors. The goal is stability over time.
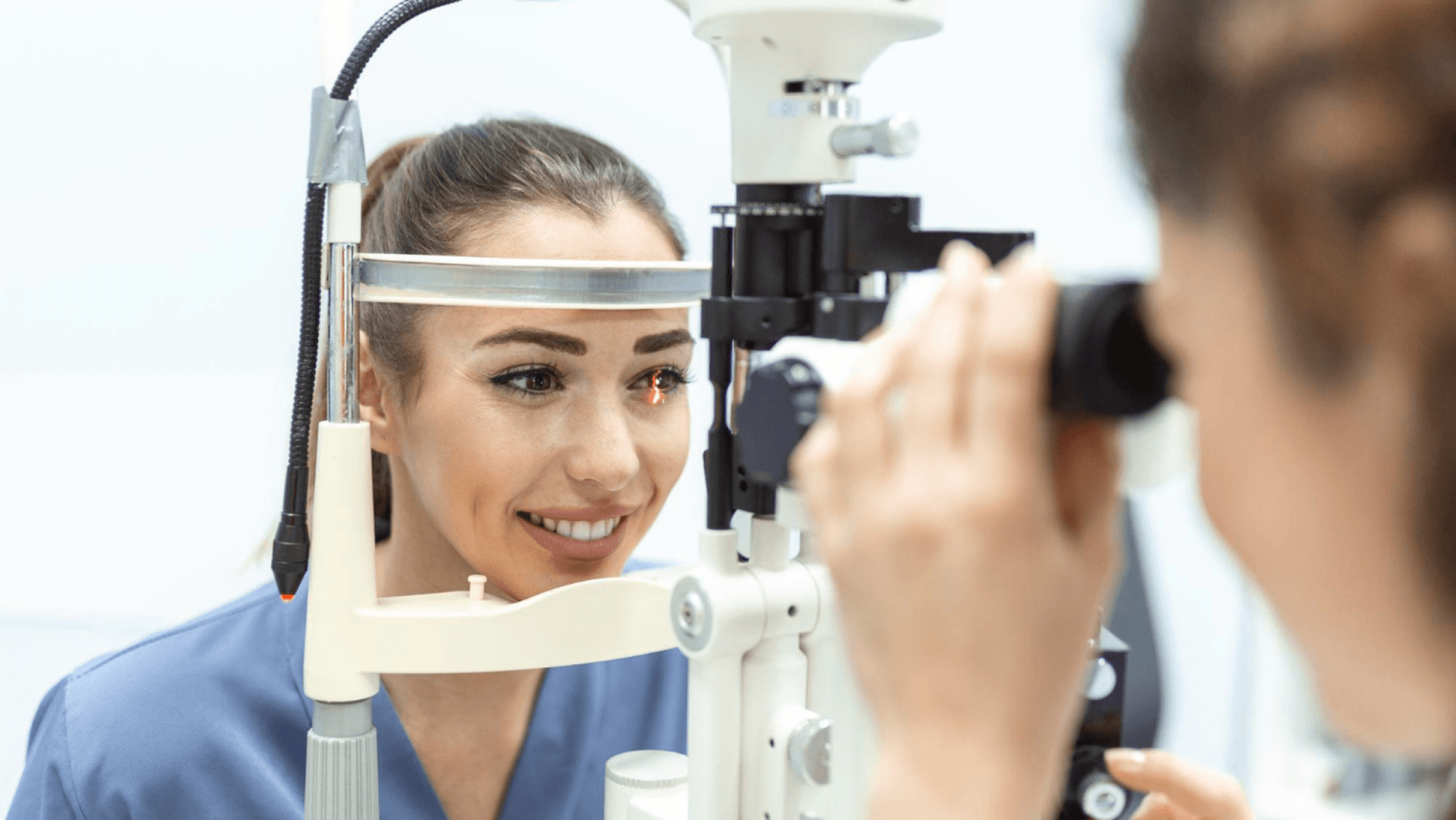
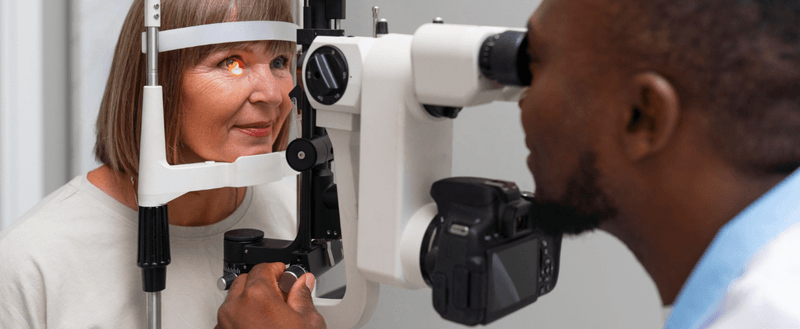
Glaucoma care is long-term. Follow-up usually includes repeat pressure checks, optic nerve review, OCT imaging, and visual field testing at intervals based on your level of risk and stability. Regular reviews help catch change early.
There is no cure, and vision that has been lost cannot be restored. Treatment is focused on preserving the vision you have and reducing the risk of further loss.
Living with glaucoma
Most people with glaucoma live full lives, but success depends on daily habits and ongoing reviews. Small practical steps can make treatment easier and more effective.
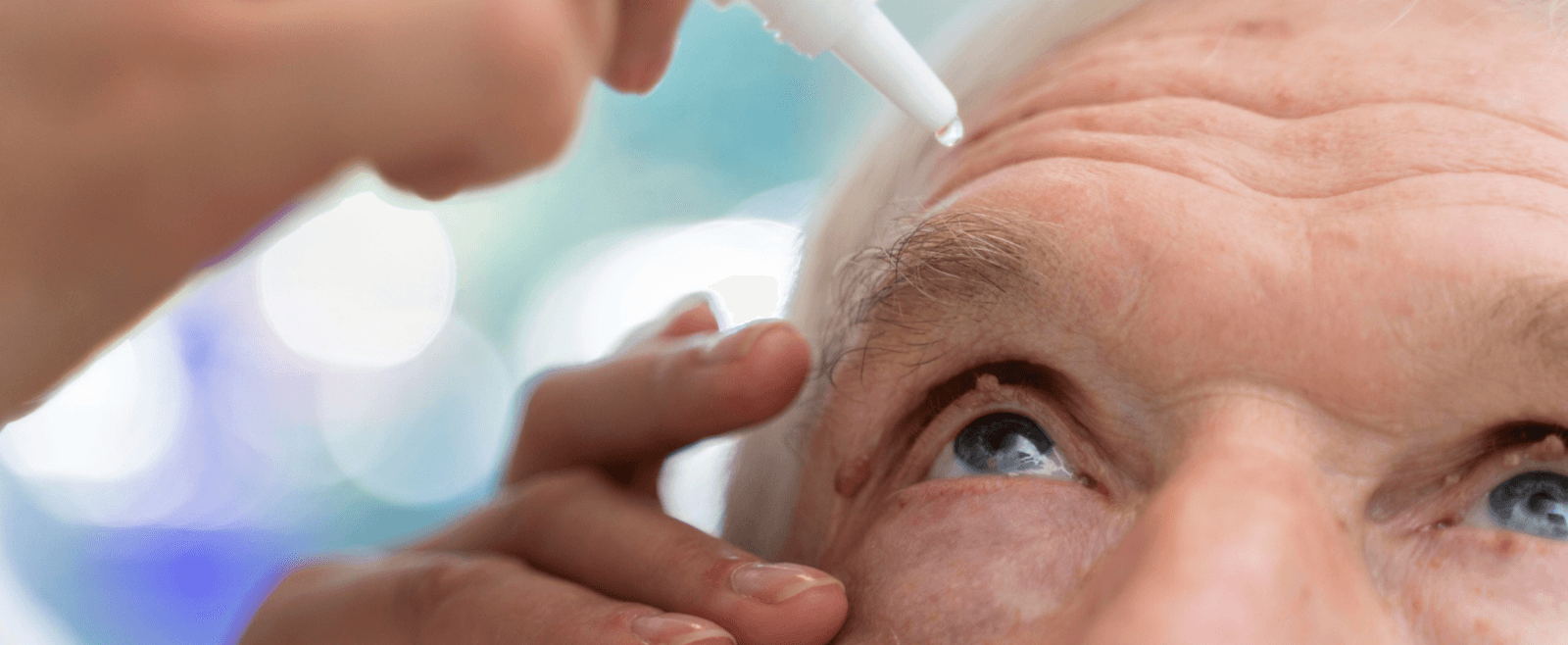
A few practical habits can make drops easier and more effective:
- Use the drop at the same time each day
- If you use more than one drop, leave a gap of a few minutes between them
- Try gentle eyelid closure after instilling drops to reduce runoff
- If you miss doses often, tell your doctor so the plan can be simplified where possible
Glaucoma can affect peripheral vision, which matters for driving safety. If you notice changes, or if you are unsure about your vision standards, discuss it early so you can get clear advice and appropriate testing.
Keep your appointments, stick with your treatment plan, and report side effects rather than pushing through them. Glaucoma is often manageable, but it relies on consistent follow-up.