Freedom from glasses starts here.
Why presbyopia happens

Presbyopia vs long sightedness
Presbyopia is an age related near blur that can affect anyone, including people who have never worn glasses. Long sightedness is a refractive error you can have at any age, and it can make near vision more difficult even before presbyopia starts. It is also common for presbyopia to sit on top of long sightedness, which is why near vision can feel like it changes quickly once your 40s arrive. If you want a clearer explanation of long sightedness, see our page on hyperopia.
When presbyopia usually starts
Most people begin to notice presbyopia in the early to mid 40s. It tends to progress gradually over the next decade or so, then stabilises later, although the pace varies from person to person.

Difficulty reading up close
Eye strain and headaches with near work
Needing brighter light
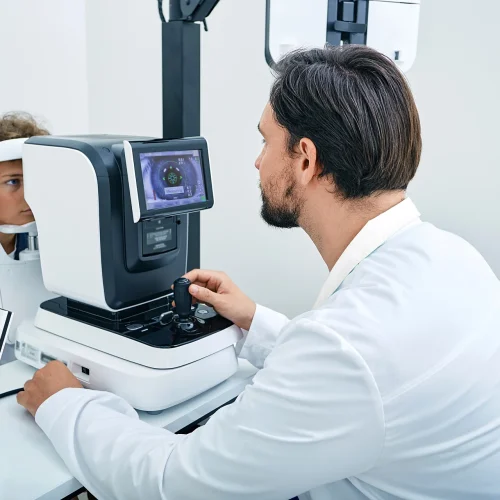
This is the natural progression of the eye’s focusing system. Most people find it gradually increases over several years. The goal of treatment is not to “stop ageing,” but to find a correction approach that fits your lifestyle and keeps day to day tasks comfortable.
A proper assessment looks at both your prescription and your eye health. That matters because not all near blur is presbyopia.
We test your near vision, assess your distance prescription, and determine what level of near support you need. This helps confirm whether simple reading glasses are enough, or whether multifocal options may suit you better.
We also check for other causes of blurred near vision, such as dry eye, early cataract changes, or retinal issues. For example, cataracts can cause haze and glare as well as blur, and dry eye can fluctuate and make focusing feel inconsistent.

There is no single best option for everyone. The right choice depends on your priorities for reading, screens, driving, hobbies, and how much you want to reduce dependence on glasses.
Reading glasses are simple and effective, especially if you only need help for occasional near tasks. Many people keep a pair for restaurants, quick reading, or short bursts of close work.
If you want one pair that works across more than one distance, multifocal or bifocal glasses can be a strong option. They can reduce the constant on and off of glasses, especially if you move between screens, paperwork, and people throughout the day.
Multifocal contact lenses aim to provide a range of vision while keeping both eyes working together. Another approach is monovision contact lenses, where one eye is set for distance and the other for near. Monovision can work well for some people, but it is not for everyone, which is why a trial is often useful. If you are exploring this approach, see our monovision page for a clear breakdown of what to expect.
The best outcomes happen when treatment matches your real world needs, not just a generic idea of “reading vision.”
Setting realistic vision goals
Before choosing an option, it helps to be clear on what matters most. Some people prioritise reading without glasses, others care most about screens and work, and many want night driving to feel sharp and comfortable. Your plan should reflect that balance.
Adapting to multifocal or monovision correction
Some options require an adaptation period. Multifocal contact lenses and monovision strategies rely on the brain learning how to use the available focus. Many people adapt over days to weeks, but it is normal to notice small compromises early, such as mild blur at certain distances or changes in contrast.
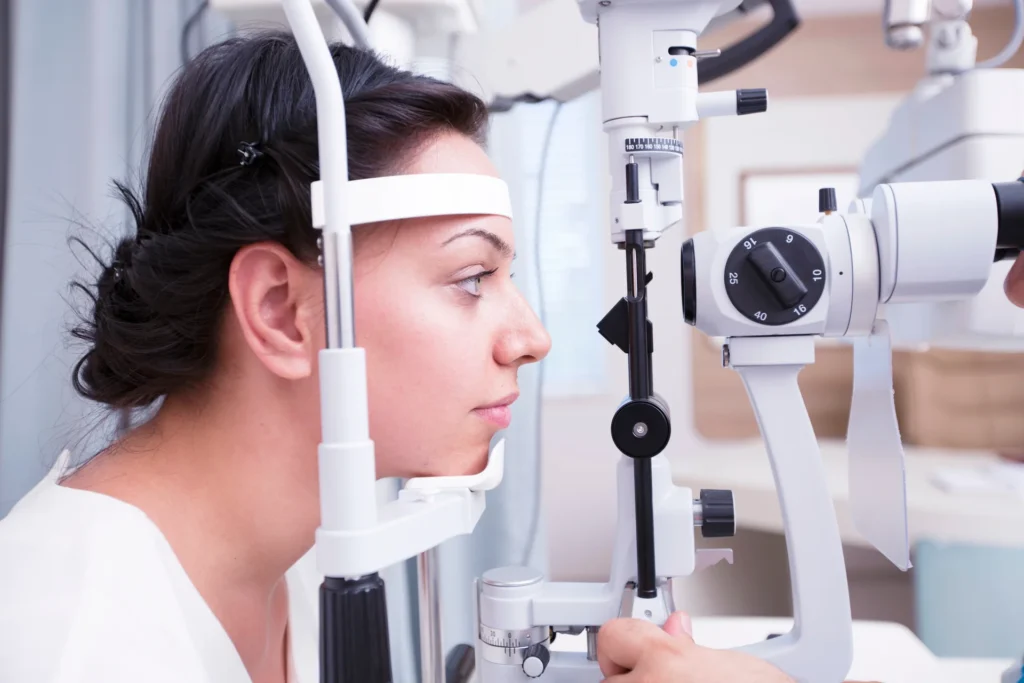
Presbyopia has multiple correction pathways, and the best plan is the one that fits your lifestyle and your eyes.
Rediscover clearer vision
Location: G11-12/566 St Kilda Road, Melbourne VIC 3004
Phone: (03) 9070 0955
Fax: (03) 9978 9426
E-mail: info@cityeyesurgeons.com.au
Copyright © 2025 City Eye Surgeons. All rights reserved. Privacy Policy.